|
I'm often asked what the difference is between the traditional method of placenta encapsulation and the holistic method (also known as the raw start method). It was finally time to make a blog post explaining the two. Clients often ask me if one is better than the other. The answer to me is - no. There is no "better" method. It can all be a matter of preference, health history and/or previous postpartum history. Both methods are great, but each method also offers a pro that you cannot get from the other.
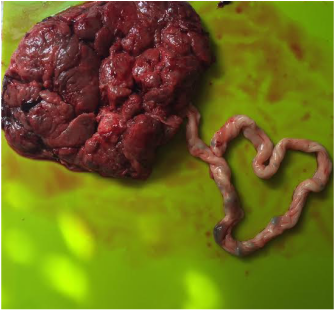
Traditional Method - The placenta is cleaned of excess blood and blood clots, then steamed in ginger, lemon & jalapeño. These are known as warming herbs postpartum in Chinese medicine. Chinese medicine says the body's energy is too cold postpartum and needs the warming energy (and raw = cold energy). It also states that steaming it makes it easier for the body to assimilate. Then the placenta is dehydrated and ground into capsules. This method usually produces less capsules than the holistic one, and is generally something that builds up slower in the body, but is meant for longer term use. The capsules keep for a very long time (some say indefinitely if you store them in the freezer for later use in life - menopause, getting your period back, stressful life events). Holistic Method - The placenta is cleaned, but not steamed at all. It gets dehydrated immediately from its raw form after I clean the excess blood and blood clots. Then it gets ground into capsules. It is not a full "raw" procedure overall, as the low temperature required in a legitimate raw foods diet is not safe for killing potential bacteria in a placenta (which is why this is called "raw start" vs "raw"). The effects can be pretty potent immediately (faster effects on energy and mood elevation, etc). They are not meant for the long term use like in the traditional method. This raw start pills usually have just 6 month shelf life if stored properly. These capsules are meant to be finished consuming faster than the traditional method. But they tend to yield more capsules since the placenta is not steamed first.
1 Comment
New research is being done on this. It seems pretty spectacular! Linked below.
"Our research is rapidly progressing. Given our recent advances, we believe that the artificial placenta may be used in premature babies in the next five years." - George Mychaliska, MD Artificial Placenta Holds Promise for Extremely Premature Infants It is difficult to accurately define delayed cord clamping when there are so many arguments on what it could mean. Some describe it as delaying for one minute, some say not until the cord stops pulsating, and others say not until the umbilical cord falls off naturally on its own (lotus birth). For the purpose of this article, let's just consider any version of delaying cord clamping (from one minute onward) as the definition, as we can begin to explore the benefits of "all of the above". So what are some benefits to delayed cord clamping? According to research, some of the top benefits are decreased risk of anemia, better outcomes for pre-term infants, increased blood volume / smoother cardiopulminary transition, increased stem cells, and neurodevelopmental benefits. Some of these benefits can be offered to infants by just waiting 60 seconds to clamp the cord. Though some disagree on the length of time needed for various reasons, including cultural tradition. Let's look at timing and benefits in more detail. 1) Decreased Risk of Anemia Delaying cord clamping by just 30 - 180 seconds after birth can result in higher hemoglobin and hematocrit during the neonatal period, increase serum ferritin levels, and reduce the incidence of iron deficiency anemia at 4-6 months of age. According to ACOG (The American Congress of Obstetrics and Gynecology), "Physiologic studies in term infants have shown that a transfer from the placenta of approximately 80 mL of blood occurs by 1 minute after birth, reaching approximately 100 mL at 3 minutes after birth. This additional blood can supply extra iron, amounting to 40–50 mg/kg of body weight. This extra iron, combined with body iron (approximately 75 mg/kg of body weight) present at birth in a full-term newborn, may help prevent iron deficiency during the first year of life." 2) Increased Blood Volume / Smoother Cardiopulminary Transition Studies have indicated that up to 1/3 of a baby's blood volume is stored in the placenta. More blood volume is not only important for higher iron stores, but also assists with healthy brain development and transition from life inside the womb. By delaying clamping, the lungs will also receive more blood, so that the exchange of oxygen in the blood can occur smoothly. Other pediatric researchers state the following: "The transition to newborn life at birth involves major cardiovascular changes that are triggered by lung aeration. These include a large increase in pulmonary blood flow (PBF), which is required for pulmonary gas exchange and to replace umbilical venous return as the source of preload for the left heart. Clamping the umbilical cord before PBF increases reduces venous return and preload for the left heart and thereby reduces cardiac output." 3) Increased Stem Cells Stem cells can develop into many different cell types in the body during early life and growth. They also have the ability to serve as a repair system, can divide without any limits in order to replenish other cells - for as long as you are still alive! They play an essential role in immune, respiratory, cardiovascular, and nervous system development (among other functions). A huge part of the argument to delay cord clamping is the fact that the concentration of stem cells in fetal blood is higher than at any other time of life. Immediate clamping of the umbilical cord leaves about 1/3 of these critical stem cells in the placenta! Many people believe that these stem cells are a birthright to newborns. 4) Neurodevelopmental Benefits There has been growing evidence about the neurodevelopmental benefits of delayed cord clamping as well. While there doesn't seem to be any difference in IQ, studies show that 4 year old children who's cords were delayed in clamping for more than 3 minutes had higher social and fine motor skills versus those who underwent clamping within 10 seconds of birth. Part of this reasoning may be due to the fact that their higher blood volume received is important for healthy brain development. 5) Better Outcomes for Pre-Term Infants Pre-term infants benefit even more in delayed cord clamping. In ten trials done on delayed cord clamping versus immediate cord clamping in pre-term infants, the benefits of delaying included reduced need for blood transfusions for low blood pressure and anemia, and a significant reduction in the incidence of intraventricular hemorrhage (brain hemorrhage). Other research has also added that delaying clamping in preemies also lowers the risk of necrotizing enterocolitis (a life threatening bowel injury). The option of delaying cord clamping is yours, and can be added to your birth plan - including many cesarean births! There are even potential options of delaying if you plan to donate or bank any cord blood (but that topic will be for another article) - although you are often still left with less of an optimal time to transfer all of the benefits to your newborn by going that route. I will leave you with the recommendations from the WHO (World Health Organization) on umbilical cord clamping:
WHO recommendations (1) In summary: Delayed umbilical cord clamping (not earlier than 1 min after birth) is recommended for improved maternal and infant health and nutrition outcomes. From 2012 WHO guidelines on basic newborn resuscitation (2): In newly born term or preterm babies who do not require positive-pressure ventilation, the cord should not be clamped earlier than 1 min after birth. When newly born term or preterm babies require positive-pressure ventilation, the cord should be clamped and cut to allow effective ventilation to be performed. Newly born babies who do not breathe spontaneously after thorough drying should be stimulated by rubbing the back 2–3 times before clamping the cord and initiating positive-pressure ventilation. From 2012 WHO recommendations for the prevention and treatment of postpartum haemorrhage 3): Late cord clamping (performed approximately 1–3 min after birth) is recommended for all births, while initiating simultaneous essential neonatal care. Early umbilical cord clamping (less than 1 min after birth) is not recommended unless the neonate is asphyxiated and needs to be moved immediately for resuscitation. Resources: http://www.who.int/elena/titles/full_recommendations/cord_clamping/en/. Optimal timing of cord clamping for the prevention of iron deficiency anaemia in infants, 2012-2014. http://www.ncbi.nlm.nih.gov/pubmed/24499758. McAdams RM, Time to Implement Delayed Cord Clamping, March 2014. http://www.ncbi.nlm.nih.gov/pubmed/23407180. Raju TN, Timing of Umbilical Cord Clamping After Birth for Optimizing Placental Transfusion, April 2013. http://www.acog.org/Resources-And-Publications/Committee-Opinions/Committee-on-Obstetric-Practice/Timing-of-Umbilical-Cord-Clamping-After-Birth. Committee Opinion, Timing of Umbilical Cord Clamping After Birth, 2014. http://archpedi.jamanetwork.com/article.aspx?articleid=2296145. JAMA Pediatrics, Andersson, Ola, MD, PhD, Lindquist, Barbro, PhD, Lindgren, Magnus, PhD, Stjernqvist, Karin, PhD, Domellöf, Magnus, MD, PhD & Hellström-Westas, Lena, MD, PhD. Effect of Delayed Cord Clamping on Neurodevelopment at 4 Years of Age A Randomized Clinical Trial, July 2015. http://www.ncbi.nlm.nih.gov/pubmed/25671807. Hooper SB, Te Pas AB, Lang J, van Vonderen JJ, Roehr CC, Kluckow M, Gill AW, Wallace EM & Polglase GR. Cardiovascular transition at birth: a physiological sequence, May 2015. http://www.scienceandsensibility.org/p/bl/et/blogid=2&blogaid=526. Sloan, Mark, MD, Common Objections to Delayed Cord Clamping - What's the Evidence Say? March 9, 2016. https://en.wikipedia.org/wiki/Stem_cell. Wikipedia, Stem Cell, April 13, 2016. http://stemcells.nih.gov/info/basics/pages/basics1.aspx. National Institutes of Health, Stem Cell Information, March 5, 2015. http://www.npr.org/sections/health-shots/2015/05/26/409697568/delayed-umbilical-cord-clamping-may-benefit-children-years-later. Haelle, Tara, NPR, Delayed Umbilical Cord Clamping May Benefit Children Years Later, May 26, 2015. http://www.ncbi.nlm.nih.gov/pubmed/24901269. Backes CH, Rivera BK, Haque U, Bridge JA, Smith CV, Hutchon DJ & Mercer JS, Placental transfusion strategies in very preterm neonates: a systematic review and meta-analysis. July 2014. http://www.ncbi.nlm.nih.gov/pubmed/25984654. Nevill E and Meyer MP, Effect of delayed cord clamping (DCC) on breathing and transition at birth in very preterm infants. July 2015. https://www.nlm.nih.gov/medlineplus/ency/article/007301.htm. Medline Plus, Intraventricular hemorrhage of the newborn, April 27, 2015. https://cord-clamping.com/2011/09/08/cesarean-delayed-clamping/. Emerson, Kate, Cesarean Section and Delayed Cord Clamping, September 8, 2011. http://fn.bmj.com/content/early/2014/12/24/archdischild-2013-305703.abstract. Hooper, Stuart B, Polglase, Graeme R & te Pas, Arjan B, A physiological approach to the timing of umbilical cord clamping at birth, December 2014. As a placenta encapsulation specialist, I am often presented with a lot of questions, myths and curiosity from either potential clients, skeptics, or just anyone wanting to know more. Here are some common myths that I have debunked for you all in one location, followed by some of my most common questions of concern.  Isn't placenta encapsulation just a form of cannibalism? Nope! While it might seem unappetizing to some people, placentophagy (the act of ingesting the placenta) is far from earning the label of cannibalism! The Merriam- Webster definition of cannibalism is "the eating of the flesh of an animal by another animal of the same kind". With placenta encapsulation, you are consuming your own placenta - and no one gets harmed in the process!  If the placenta is a filter for the baby, isn't it full of toxins? "Filter" is often the term given to placentas. However, placentas don't function in the same way that a filter for something like a furnace would. Placentas can prevent toxins from reaching the fetus - but they don´t continue to store all of the things that we don´t want for the maternal body or baby. The placenta allows nutrients to pass through the fetus, keeps the maternal and fetal blood separated, and allows for gas exchanges to occur. Waste and toxins are processed by the liver and kidneys of the pregnant body and eliminated.  I'm vegetarian/vegan. I can't eat my placenta. Isn't it meat? Placentas are the only meat that come from life, not death. This makes it totally suitable for vegans and vegetarians. I myself am a vegetarian, and I did placenta encapsulation after the birth of my son. If it isn't kept for consumption or some sort of ritual, the placenta will likely get incinerated - which is more wasteful than doing something with this nutrient rich organ! Don't all of the nutrients just get cooked out? There is no actual high heat cooking that is done during the process of placenta encapsulation. The Traditional Chinese Method uses steaming and dehydrating, and the raw method eliminates the steaming step of the process. A study was performed on heat-dried placentas that showed they still contained nutrients such as fiber, protein, hormones, and high mineral levels (particularly sodium, potassium, and phosphorous). Don't animals only eat their placenta to avoid attraction of predators? There is no hard evidence that this is the only case for mammalian placenta consumption in the wild. While this may be part of the reason placentophagy is practiced by almost all mammals, there have also been studies indicating that placenta consumption by mammals in the wild assists with pregnancy induced analgesia, increased lactation, and a better outcome in mother-baby interaction and caretaking. Can I still encapsulate if I received medical interventions (epidural, pitocin, cesarean, I am GBS+, or I have pre-eclampsia)? Will the hospital release it to me? Yes to all of it! The drugs used in these procedures (epidurals and pitocin) actually break down fairly quickly after entering the bloodstream. I have encapsulated for numerous clients who have received these interventions, and have never had a negative report post-encapsulation. Group B strep is a naturally occurring bacteria that rarely has any health threat. Any possible bacteria will get killed during the steaming and/or heat of the dehydration process during encapsulation. If this did develop into an infection during labor, then your placenta would not be suitable for encapsulation (and likely sent to pathology). Pre-eclampsia is not automatically contraindicated for placenta encapsulation. Many clients with pre-eclampsia have successfully consumed their placenta capsules. As long as no problem or infection is noted during the placenta examination, the placenta will likely be released to you and suitable for encapsulation. The hospitals in the Seattle area are very familiar with placenta encapsulation, and I have never had a problem obtaining a healthy placenta from anywhere. They will ask you to fill out a release form. Always let your midwife/OB and all staff know that you intend to keep your placenta! I hear there are no studies. What are the benefits of encapsulation? Most of the information gathered on placenta encapsulation has been done through anecdotal evidence provided by those who consumed their placenta postpartum. Some of the main positive side effects reported have been: reduction in postpartum baby blues, increased lactation, reduction in postpartum bleeding, reduction in postpartum pain, increased energy, and faster healing. There have been small studies performed showing a positive responses for placentas as a lactagogue, as well as some studies on placenta analgesia. We also know that the placenta contains amazing nutrients, minerals, and hormones such as progesterone, estrogen, oxytocin, placental opioid-enhancing factor, human placental lactogen, iron, corticotropin-releasing hormone, urokinase inhibiting factor, factor XIII, protein, fiber, and potassium (to name a few) - all of which aid in the listed benefits to placenta encapsulation. How do I know that my placenta will not get mixed up with someone else's? This is something that I take very seriously! For starters, I only work on one placenta at a time, and I label everything throughout the process. There is rarely more than one placenta in my home at a time. But if that happens, I don't even get to the second placenta until the first one is 100% completed. You also have the option of signing over a release to me in which your placenta gets a color coded and initialed label beginning as soon as I pick it up. I have my placenta in the freezer. Can I still have it encapsulated? As long as your placenta meets a few conditions, it will still be totally suitable for encapsulation. 1. It needs to have been frozen within 48-72 hours after the birth (and refrigerated before that). 2. It generally shouldn't be frozen for more than 6-12 months (ideally no longer than 6 months). 3. There should be no signs of frostbite existing on the placenta. 4. It was never thawed and then re-frozen. What happens if there is an infection and/or my placenta needs to be sent to pathology? If there is no risk of infection, but the hospital staff wants to send the placenta to pathology anyway, ask them if it is possible to just take a small portion instead of the entire placenta. However, if you develop an infection during labor, if there is an infection in the placenta, and/or the placenta needs to be sent to pathology for any other medical reason, it becomes unsuitable for encapsulation. The proper handling of the placenta cannot be guaranteed and monitored once sent to pathology, and there are safety concerns with ingesting a placenta that may contain an infection. References:
Nikole Keller, (August 7, 2015). Uncovering the Truth About Bacteria and Heavy Metals in the Placenta (Online) http://www.ncbi.nlm.nih.gov/pubmed/10932499. Nutrients and hormones in heat-dried human placenta, June 2000. Mark B. Krystal, Jean M. DiPirro & Alexis C. Thompson, (May 25, 2012). Placentophagia in Humans and Nonhuman Mammals: Causes and Consequences, Ecology of Food and Nutrition, 51:3, 177-197. http://www.acsu.buffalo.edu/~kristal/placentophagia%20review.pdf. http://www.drugs.com/pro/pitocin.html. Drugs.com, October 2015. Ilona S. Yim, PhD, Laura M. Glynn, PhD, Christine Dunkel Schetter, PhD, Calvin J. Hobel, MD, Aleksandra Chicz-DeMet, PhD & Curt A. Sandman, PhD, (October 27, 2009). Elevated Corticotropin-Releasing Hormone in Human Pregnancy Increases the Risk of Postpartum Depressive Symptoms. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2768579/ Lisa M. Bodnar, PhD, MPH, RD, Mary E. Cogswell, DrPh, RN & Thad McDonald, MD, (July 2005). Have we forgotten the significance of postpartum iron deficiency? Volume 193, Issue 1, Pages 36-44. http://www.ajog.org/article/S0002-9378(04)02092-7/abstract. Kristal MB, (1991). Enhancement of Opioid-Mediated Analgesia: A Solution to the Enigma of Placentophagia. http://www.ncbi.nlm.nih.gov/pubmed/1956610. Soykova-Pachnerova, Eva, Brutar, Vlastimil, Golova, Berta & Zvolska, Eva, (December 5, 2006). Placenta as a Lactogogon. First Obstetric Clinic. https://mommyfeelgood.files.wordpress.com/2010/10/placenta_lactagogon1.pdf  I had an incredible time educating the public at the table I had for my business, Seattle Placenta Encapsulation, at Babyfest NW this month. Placentas are a part of my everyday life, and at this point, I even meet people never intending on having children who have heard of this service. But that Saturday helped me realize that there are still a large number of people in the surrounding Seattle region who are unaware that this exists. I heard a mix of everything that day. Stories of families wishing they had encapsulated their placentas, stories of hospitals that "forgot" to save the placenta for the mother, and a lot of "I've heard about this. My good friend did this and said it was awesome!" And on the opposite end, I sure got my fair share of "So what is placenta encapsulation?" I respond with a breakdown of what it means, and I get "Ew! No thanks, I'm good!" Here's the thing - I'm not in this business to "make" anyone do anything. Yes, I'm incredibly passionate about this work. I love it, I honor it, I believe in it. I have my own personal experience that did wonders for me, and I hear from clients all the time about how much this service has helped their transition in the postpartum world. However, I understand that this is not the most comfortable treatment for everyone, and I'm all about empowering families. I love to educate people about what I do, and why I do it. But I'm not going to pressure you to come to my table as you walk by hesitantly at a birth fair - I do not like "salespeople" pressure put on me. That being said, I hear so often from my clients, "You need to get out there and tell people your services exist! I found out about you so last minute, and I'm so glad I did!" So where do I find the balance between sharing my resources with the consumers of the birthing world, while being empathetic and maintaining appropriate boundaries? How would you prefer to hear about placenta services? |
AuthorWrite something about yourself. No need to be fancy, just an overview. Archives
February 2017
Categories |











 RSS Feed
RSS Feed
